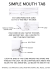Clinical/Scientific Notes Paraneoplastic encephalomyelitis
Transcription
Clinical/Scientific Notes Paraneoplastic encephalomyelitis
Clinical/Scientific Notes Paraneoplastic encephalomyelitis associated with pancreatic tumor and anti-GAD antibodies L. Hernández-Echebarrı́a, MD; A. Saiz, MD; A. Arés, MD; J. Tejada, MD; L. Garcı́a-Tuñón, MD; C. Nieves, MD; and F. Graus, MD Glutamic acid decarboxylase (GAD), the enzyme that catalyzes the conversion of glutamate to ␥-aminobutyric acid (GABA), is expressed in GABA-secreting neurons and pancreatic  cells.1 Anti-GAD antibodies (GAD Abs) have been described in patients with type 1 diabetes mellitus and patients with two CNS disorders, stiff-person syndrome and cerebellar ataxia associated with polyendocrine autoimmunity.2 We report a patient with paraneoplastic encephalomyelitis associated with a pancreatic tumor and GAD Abs. Case report. A 67-year-old man presented paresthesias and numbness in hands, feet, and perioral region. Over the next 2 weeks, he developed gait instability that required bilateral support for walking. The general examination was unremarkable. The neurologic examination showed gaze-evoked downbeat nystagmus. Deep tendon reflexes were absent in the legs. There was hypoesthesia in glove and stocking distribution, with decreased vibration and joint position sense in the fingers and toes. He showed truncal and gait ataxia and moderate limb dysmetria. Routine hematologic and biochemical analysis were normal. CSF analysis revealed a protein level of 314 mg/dL, 11 lymphocytes/ mm3, and negative oligoclonal IgG bands. Serum and CSF serologies and cultures ruled out an infectious etiology. Antineuronal antibodies (Hu, Yo, Ri, Ma 1 and 2, CV2, and amphiphysin antibodies) were negative, but GAD Abs, detected by immunohistochemistry and RIA,2 were present in serum (1/80,000) and CSF (1/800). No other autoantibodies were detected either by immunohistochemistry or immunoblot of neuronal extracts. Nerve conduction studies demonstrated absent sensory nerve action potential in the legs with normal motor nerve and F-wave studies. Brain MRI was normal. A CT scan of the abdomen demonstrated a mass (5.5 ⫻ 3 ⫻ 5 cm) in the body of the pancreas without evidence of metastasis. The patient underwent a resection of the corpus and cauda of the pancreas combined with splenectomy. A histopathologic examination revealed a neoplasm of the pancreatic body, which showed an intense infiltration of inflammatory cells (figure) and a positive immunostaining for synaptophysin and chromogranin A. The tumor was classified as a well-differentiated, nonfunctioning pancreatic endocrine neoplasm. Symptoms worsened over the ensuing months. He also developed painful spasms in the left leg with fixed dorsiflexion posture of the foot. A new electromyogram demonstrated persistent motor activity in the left leg. Symptoms did not improve after several courses of IV immunoglobulins; he developed confusion and agitation and died from aspiration bronchopneumonia. The expression of GAD antigen by the patient’s tumor was demonstrated by the characteristic immunoreactivity of the tumor cells after incubation with GAD-6 monoclonal antibody (Hybrioma Bank, Iowa City, IA) (see figure) or biotinylated IgG of a patient with high titers of GAD Abs. Specificity of staining for GAD antigen was confirmed by competition experiments in which binding of the GAD-6 monoclonal antibody was blocked by preincubation of tumor sections with a human serum with high titers of GAD Abs (see figure) but not with serum from a normal individual (not shown). At brain autopsy, the CNS appeared grossly normal. Microscopically, there was an extensive loss of Purkinje cells in the cerebellum and proliferation of Bergmann astrocytes. A vacuolization in the posterior columns of the spinal cord was also noticeable. Inflammatory infiltrates were not detected in the cerebellum or other areas of the nervous system. Discussion. The current study shows that GAD Ab response can be associated with tumors other than thymoma.3 This finding is important because the presence of GAD Abs is usually associated with the nonparaneoplastic form of the stiff-person syndrome and in the cerebellar ataxia associated with polyendocrine autoimmunity, which are unrelated to malignancies with the exception of thymoma.1,2,4,5 The detection of high titers of GAD Abs in a patient with a neurologic syndrome usually indicates that the probable cause is nonparaneoplastic autoimmunity, and the search for an underlying cancer is unnecessary. Although this statement is probably correct when the patient has a stiff-person or cerebellar syndrome,1,2 in the clinical setting of a possible encephalomyelitis, a possible paraneoplastic origin should be considered even if the patient has GAD Abs.6 The pathogenic role of GAD Abs in the two characteristic neurologic disorders, stiff-person and cerebellar ataxia, has been questioned because GAD is a cytoplasmic antigen.7 In our patient, the massive infiltration of the tumor by T lymphocytes suggests that the GAD expression by the tumor could induce a complex (humoral and cellular) immune response, initially driven to control the tumor growth and later misdirected to the nervous system. The final mechanisms of neuronal damage are unclear, but it was probably caused by a T cell–mediated immune attack against GAD-positive neurons.6 From the Neurology (L.H.-E., A.A., J.T., L.G.-T.) and Pathology (C.N.) Services, Hospital de León, and Neurology Service (A.S., F.G.), Institut d’Investigació Biomédica August Pi i Sunyer, Hospital Clı́nic, University of Barcelona, Spain. Disclosure: The authors report no conflicts of interest. Received April 18, 2005. Accepted in final form October 21, 2005. Address correspondence and reprint requests to Dr. L. HernándezEchebarrı́a, Neurology Service, Hospital de León, Altos de Nava s/n, 24071 León, Spain; e-mail: [email protected] Copyright © 2006 by AAN Enterprises, Inc. References 1. Solimena M, Folli F, Aparisi R, Pozza G, De Camilli P. Autoantibodies to GABA-ergic neurons and pancreatic beta cells in stiff-man syndrome. N Engl J Med 1990; 322: 1555–1560. 2. Saiz A, Arpa J, Sagasta A, et al. Autoantibodies to glutamic acid decarboxylase in three patients with cerebellar ataxia, late-onset insulindependent diabetes mellitus, and polyendocrine autoimmunity. Neurology 1997;49:1026–1030. 3. Vernino S, Lennon VA. Autoantibody profiles and neurological correlations of thymoma. Clin Cancer Res 2004; 10: 7270–7275. 4. Meinck H-M, Faber L, Morgenthaler N, et al. Antibodies against glutamic acid decarboxylase: prevalence in neurological diseases. J Neurol Neurosurg Psychiatry 2001;71:100–103. Figure. (A) Tumor section immunostained with a monoclonal antibody against CD3 antigen (T lymphocytes) shows a massive infiltration of T lymphocytes around tumor cells. (B) Incubation of the section with glutamic acid decarboxylase-6 monoclonal antibody demonstrates positive staining of tumor cells. (C) Glutamic acid decarboxylase-6 immunoreactivity is abolished by preincubation with the patient’s serum. Counterstained with hematoxylin and eosin; ⫻100 (A); ⫻200 (B, C). 450 NEUROLOGY 66 February (1 of 2) 2006 5. Barker RA, Revesz T, Thom M, Marsden CD, Brown P. Review of 23 patients affected by the stiff man syndrome: clinical subdivision into stiff trunk (man) syndrome, stiff limb syndrome, and progressive encephalomyelitis with rigidity. J Neurol Neurosurg Psychiatry 1998;65:633– 640. 6. Darnell RB, Posner JB. Paraneoplastic syndromes involving the nervous system. N Engl J Med 2003;349:1543–1554. 7. Dalakas MC, Li M, Fujii M, Jacobowitz DM. Stiff person syndrome: quantification, specificity, and intrathecal synthesis of GAD65 antibodies. Neurology 2001;57:780–784. Lower motor neuron weakness after diving-related decompression Our patient’s hand weakness is explained by infarction involving the anterior horn cells in the spinal cord due to diving-related decompression. Spinal cord damage following diving is recognized,1-5 but our case is unusual because of the cervical cord involvement with lower motor neuron weakness of the upper limb, in contrast to the more typical thoracic spinal cord involvement with upper motor neuron weakness of the lower limbs and sensory loss.1-3 In our case, this presentation had led to the initial diagnosis by a neurologist of ALS. Spinal cord infarction is usually reported with type II decompression sickness1 but can occur in the absence of clinical signs of decompression sickness.5 In a study of goats with different diving exposures, the presence of spinal cord lesions did not correlate with the typical features of decompression sickness.5 Spinal cord involvement may occur following dives conducted in accordance with US Navy decompression tables.1,4 Rapid ascent has been associated with spinal cord involvement.1,5 The most likely mechanism responsible for decompressionrelated myelopathy is spinal cord ischemia due to congestion of the epidural vertebral venous system by nitrogen gas bubbles. The epidural vertebral venous system (Batson plexus) can be obstructed by gas bubbles that collect, coalesce, and grow, when other major veins do not become obstructed, because the system functions as a valveless relatively stagnant venous lake in which the direction of flow changes frequently, in contrast to the unidirectional conduit function of other veins.6 In addition to mechanically obstructing venous outflow, gas bubbles in the venous bed may accelerate coagulation, leading to more complete venous obstruction.6 Robert D. Henderson, FRACP; and Michael P. Pender, MD Myelopathy is a recognized complication of diving and usually presents with upper motor neuron weakness and sensory loss of the lower limbs due to thoracic spinal cord damage.1,2 Here we present a case of lower motor neuron upper limb weakness due to infarction of the anterior horn cells of the spinal cord following diving. To our knowledge, this is the first report of an isolated lower motor neuron syndrome following diving-related decompression. A 46-year-old woman was referred for electromyography (EMG) with a clinical diagnosis of ALS. Two months earlier, she had noted weakness in her right hand without sensory symptoms. The patient was a recreational scuba diver and recalled diving to 90 ft, 1 week prior to the onset of weakness. She ascended quickly but not in violation of her diving table and 20 hours later took an international flight. There was no significant past medical history. On examination, there was wasting of the small muscles of the right hand and a prominent inability to extend the right middle finger. Scattered fasciculations were seen in the small muscles of the right hand. There was mild weakness of right elbow extension, forearm pronation, wrist extension and thumb abduction, and moderate weakness of finger extension and abduction. Left finger abduction was mildly weak, but power was otherwise normal in the left upper limb. The biceps, supinator, and triceps jerks were normal bilaterally. The upper limb sensation, cranial nerves, and lower limb examination were normal. Nerve conduction studies showed low amplitude right ulnar and median compound muscle action potentials (CMAPs) with normal conduction velocities, F waves, and corresponding sensory studies. No conduction block was present. The right radial CMAP recording over the extensor digitorum was normal. The EMG showed fibrillations and fasciculations in the right first dorsal interosseous and opponens pollicis muscles with reduced recruitment of complex large motor units. There was increased size of motor units in the right deltoid, triceps, pronator teres, and lower cervical paraspinal muscles. Large motor units were also present in the left first dorsal interosseous and opponens pollicis muscles. MRI of the cervical spine at the time of the clinical examination showed increased signal in the spinal cord from C3 to C7 vertebral bodies on sagittal T2 imaging. On T2 axial cuts, the increased signal was predominantly in the right anterior horn, with hypointensity on T1 imaging (figure). T2 hyperintensity was also present to a lesser extent in the left anterior horn. No enhancement occurred following the injection of gadolinium. The MRI was consistent with focal infarction of the cervical spinal cord. On follow-up, 4 months after the onset of weakness, her neurologic condition was unchanged. From the Department of Neurology, Royal Brisbane and Women’s Hospital, School of Medicine, University of Queensland, Australia. Disclosure: The authors report no conflicts of interest. Received August 25, 2005. Accepted in final form October 25, 2005. Address correspondence and reprint requests to Dr. R.D. Henderson, Department of Neurology, Royal Brisbane and Women’s Hospital, Butterfield St., Herston, 4029, Queensland, Australia; e-mail: Robert_Henderson@ health.qld.gov.au Copyright © 2006 by AAN Enterprises, Inc. References 1. Kimbro T, Tom T, Neuman T. A case of spinal cord decompression sickness presenting as partial Brown–Sequard syndrome. Neurology 1997;48:1454–1456. 2. Hierholzer J, Tempka A, Stroszczynski C, et al. MRI in decompression illness. Neuroradiology 2000;42:368–370. 3. Manabe Y, Sakai K, Kashihara K, Shohmori T. Presumed venous infarction in spinal decompression sickness. AJNR Am J Neuroradiol 1998;19: 1578–1580. 4. Aharon-Peretz J, Adir Y, Gordon CR, Kol S, Gal N, Melamed Y. Spinal cord decompression sickness in sport diving. Arch Neurol 1993;50:753– 756. Figure. (A) Axial T2 MRI of the spine at C3 to C4 level with hyperintensity of the right anterior horn and to a lesser extent of the left anterior horn. (B) Corresponding T1 scan showing hypointensity of the right anterior horn consistent with infarction. February (1 of 2) 2006 NEUROLOGY 66 451 5. Blogg SL, Loveman GA, Seddon FM, et al. Magnetic resonance imaging and neuropathology findings in the goat nervous system following hyperbaric exposures. Eur Neurol 2004;52:18–28. 6. Hallenbeck JM, Bove AA, Elliott DH. Mechanisms underlying spinal cord damage in decompression sickness. Neurology 1975;25:308–316. Cortical liquefaction in severe human herpesvirus 6 encephalopathy and 5, resulting in laminar necrosis.2,3 It is histologically defined as pan-necrosis, that is, the death of neurons, glia, and blood vessels with resultant denatured proteins, reactive gliosis, and deposition of fat-laden macrophages.3 On MRI, cortical laminar necrosis is seen as high intensity both on T1-weighted and FLAIR images.2,4 Though the exact mechanism of T1 shortening in laminar necrosis is still uncertain, it is postulated to reflect the presence of denatured protein and fat-laden macrophages.2,4 Cortical lesions were not reported to manifest low signal intensity at any stage of cortical laminar necrosis on either T1-weighted and FLAIR images.4 Therefore, the appearance of the cortical lesions in this case is distinct from cortical laminar necrosis as reported in the literature. What is the mechanism by which the cortex liquefied in this patient? Histopathologic studies in patients with severe perinatal asphyxia have revealed that cortical injuries generally involve all layers of the cerebral cortex and are only occasionally laminar.5 In addition, intracortical fibers do not seem to be myelinated in neonates or young infants, as staining with Luzon fast blue (for evaluation of myelination) does not appear until after 12 months.6 The absence of myelin might make the cortex more likely to liquefy, as myelin gives stability to the axons and also nourishes them.7 Thus, one explanation might be that liquefaction results from the different pattern of cortical involvement and the absence of intracortical myelin in this 9-month-old infant. However, the fact that cortex does not liquefy after arterial infarction at this age makes this explanation unlikely. Another possibility is that HHV6 might directly affect neurons, astrocytes, and macrophages.1 By the effects on astrocytes and macrophages, the virus might reduce reactive gliosis and the deposition of fat-laden macrophages that cause T1 shortening in cortical laminar necrosis. In any case, further study and further cases will be needed to determine the clinical significance of this severe liquefactive change and the factors causing it. J. Takanashi, MD; A.J. Barkovich, MD; H. Tada, MD; N. Takada, MD; K. Fujii, MD; and Y. Kohno, MD Human herpesvirus 6 (HHV6) is the causative agent of the common childhood infectious disease exanthema subitum. Primary infection of CNS by HHV6 can cause seizures and encephalitis/ encephalopathy.1 We report a 9-month-old girl with severe HHV6 encephalopathy, in whom a subacute MRI showed an unusual appearance of the cerebral cortex suggesting cortical liquefaction. Case report. A previously healthy 9-month-old Japanese girl was admitted because of status epilepticus for 1 hour following a 1-day prodromal illness consisting of fever (around 38.5 °C for 3 days) and vomiting. After her seizure was controlled, she was in a comatose state and required intubation. Laboratory examination revealed elevated serum liver enzyme activities. CSF showed normal cell count (1/mm3), protein level (18 mg/dL), and glucose level (122 mg/dL). EEG showed polyspikes in bilateral centroparietal regions. HHV6 was later isolated from her throat swab and serum, and a diagnosis of HHV6 encephalopathy was established. Clinical symptoms or laboratory data suggesting hemorrhagic shock and encephalopathy syndrome (shock, diarrhea, disseminated intravascular coagulation or renal dysfunction) were not observed. A faint skin rash appeared on her body on the 5th day. She was treated with methylprednisolone (30 mg/kg/day for 3 days) and acyclovir. Her liver function gradually normalized within a month. Her consciousness level gradually improved, but she was discovered to have severe psychomotor retardation and tetraplegia. MRI on the 40th day demonstrated marked T2 prolongation of the frontal and occipital cortex overlying the abnormally high intensity white matter (figure, A). The abnormal cortex was of homogenously low signal intensity in its deeper layers with its more superficial layers demonstrating isointensity to the remainder of the cortex on T1-weighted and fluid-attenuated inversion recovery (FLAIR) (figure, B) images. T1 shortening and T2 prolongation in the corpus striatum and cerebral atrophy were seen. Discussion. Markedly high signal intensity on T2-weighted images and low signal intensity on T1-weighted and FLAIR images would imply liquefactive changes within the cortex. A search of the literature has revealed no report of apparent cortical liquefaction in patients with encephalopathy or infarction. Histologic and animal studies have demonstrated much more vulnerability of gray matter than white matter to hypoxic– ischemic insults. Of the six cortical layers, layers 3 and 5 are the most vulnerable; layers 2 and 4 are more resistant. Therefore, neuronal damage has a tendency to occur especially in layers 3 Acknowledgment The authors thank Dr. Masaharu Hayashi (Department of Clinical Neuropathology, Tokyo Metropolitan Institute for Neuroscience, Tokyo, Japan) for comments. From the Department of Pediatrics (J.T., H.T., N.T., K.F., Y.K.), Graduate School of Medicine, Chiba University, and Department of Pediatrics (J.T.), Kameda Medical Center, Kamogawa, Japan; and Neuroradiology Section (A.J.B.), Department of Radiology, University of California San Francisco. Disclosure: The authors report no conflicts of interest. Received June 7, 2005. Accepted in final form October 25, 2005. Address correspondence and reprint requests to Dr. J.-I. Takanashi, Department of Pediatrics, Kameda Medical Center, 929 Higashi-cho, Kamogawashi, Chiba 296-8602, Japan; e-mail: [email protected] Figure. (A) T2-weighted image (4,000/ 100 milliseconds repetition/echo time) on 40th day demonstrated marked T2 prolongation of the frontal and medial parietal and occipital cortex (arrows). (B) Sagittal fluid-attenuated inversion recovery images (10,000/110 milliseconds, 2,200 inversion time) show low intensity of the deeper layers of the frontal cortex (arrow) but normal intensity of the most superficial portions of the cortex. 452 NEUROLOGY 66 February (1 of 2) 2006 Copyright © 2006 by AAN Enterprises, Inc. References 1. Yoshikawa T, Asano Y. Central nervous system complications in human herpesvirus-6 infection. Brain Dev 2000;22:307–314. 2. Siskas N, Lefkopoulos A, Ioannidis I, Charitandi A, Dimitriadis AS. Cortical laminar necrosis in brain infarcts: serial MRI. Neuroradiology 2003;45:283–288. 3. Boyko OB, Burger PC, Shelburne JD, Ingram P. Non heme mechanism for T1 shortening: pathologic, CT, MR elucidation. AJNR Am J Neuroradiol 1992;13:1439–1445. 4. Komiyama M, Nakajima H, Nishikawa M, Yasui T. Serial MR observation of cortical laminar necrosis caused by brain infarction. Neuroradiology 1998;40:771–777. 5. Hopkins IJ, Farkas-Bargeton E, Larroche JC. Neonatal neuronal necrosis: its relationship to the distribution and maturation of oxidative enzymes of newborn cerebral and cerebellar cortex. Early Hum Dev 1980; 4:51–60. 6. Iai M, Yamamura T, Takashima S. Early expression of proteolipid protein in human fetal and infantile cerebri. Pediatr Neurol 1997;17:235– 239. 7. Barkovich AJ. Magnetic resonance techniques in the assessment of myelin and myelination. J Inherit Metab Dis 2005;28:311–343. Glomeruloid hemangiomas: A marker for POEMS Tracy Weimer, MD; Amy Norton, MD; and Ludwig Gutmann, MD Polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes (POEMS) is a multisystem syndrome that may accompany plasma cell dyscrasias.1,2 Polyneuropathy and a monoclonal plasmaproliferative disorder must be present along with one other minor criterion, including sclerotic bone lesions, Castleman’s disease, organomegaly, edema, endocrinopathy, skin changes, or papilledema. Other associated findings may include ascites, pleural effusions, and thrombocytosis. We describe a patient with glomeruloid hemangiomas, a skin abnormality seen exclusively in POEMS.3,4 This has been reported only rarely in the neurologic literature and is a useful diagnostic criterion.5 Case report. A 58-year-old woman presented with weakness, distal sensory loss, pain, and edema in the lower extremities. The symptoms had progressed over 3 years. She was using a walker to ambulate. Neurologic examination 3 years earlier, at the time of an episode of low back pain, was normal. She was an obese woman with extensive edema of the extremities and thickening of the skin in the legs and forearms. Muscle strength was 4-/5 in the arms and legs except distally in the legs where no motor function was present. Vibration was moderately decreased in the hands and absent in the feet. Position sense, pin, and temperature were moderately decreased in the feet. All reflexes were absent. Bulbar strength was normal. Laboratory studies revealed an elevated TSH of 8.45. Serum protein electrophoresis was consistent with a monoclonal gammopathy and immunofixation revealed monoclonal IgA lambda M-protein. Initial skeletal survey was negative. CT of the chest/ abdomen/pelvis showed scattered lymph nodes, which failed to meet size criteria for lymphadenopathy. Bone marrow biopsy showed 5% plasma cells and normoblastic maturation. Nerve conduction/EMG studies on both median and ulnar nerves showed prolonged distal motor latencies ranging from 6.9 to 9.5 m/sec (normal 4.2) and slowed velocities ranging from 17.8 to 23.1 m/sec (normal greater than 45 m/sec). All sensory nerve action potentials were absent. Many fibrillations were seen in distal and proximal muscles of the legs and distally in the arms. Motor unit potentials were decreased or absent in legs. The patient was treated with five courses of IV immunoglobulin (IVIg) with some mild subjective improvement of the distal extremity pain. Despite treatment with IVIg, she was dramatically worse 4 months later. Weakness was severe distally in the legs and moderate in the arms. Reflexes remained absent. At this follow-up visit, erythematous papules were noted across the abdominal skin. Skin biopsy was performed on these lesions and revealed a glomeruloid hemangioma (figure). A repeat skeletal survey revealed a previously unseen area of sclerosis in the right fourth rib. The sclerotic lesion was biopsied and revealed a small area of plasma cell proliferation. Discussion. The cardinal features of POEMS include a polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes. The sensorimotor polyneuropathy is generally the presenting complaint in POEMS syndrome. It usually has both demyelinating and axonal features and is slowly progressive and debilitating in most cases. The monoclonal (M) protein abnormality consists of IgA or IgG Figure. Microscopic section showing glomeruloid hemangioma stained with hematoxylin and eosin. Insert shows hemangioma on abdominal wall. heavy chains with lambda light chains. Anti-myelin-associated glycoprotein antibodies are not present in POEMS as it is in many IgM paraproteinemias. Bone lesions, when present, are usually sclerotic. In cases of POEMS associated with solitary osteosclerotic lesions, improvement of all symptoms is seen after irradiation or surgical excision of the lesion. The skin changes may consist of hyperpigmentation, hypertrichosis, hyperhidrosis, skin thickening, and hemangiomas. Endocrinopathies includes diabetes, impotence, gynecomastia, and hypothyroidism. Organomegaly may be hepatosplenomegaly or lymph node enlargement. Approximately 60% of biopsies of enlarged lymph nodes show histopathology similar to that seen in Castleman’s disease (angiofollicular lymph node hyperplasia, vascular proliferation, sinusoidal histiocytes, and sheets of plasma cells).6 The patient described in this report fulfills the criteria for a diagnosis of POEMS. Her polyneuropathy showed evidence of demyelination and axonal degeneration. She had an osteosclerotic myeloma and an IgA lambda M-protein. Hypothyroidism and marked peripheral edema were present. Skin changes included marked thickening and glomeruloid hemangiomas. Glomeruloid hemangiomas are a unique skin abnormality in POEMS, present in as many as 24 to 44% of patients.7 These appear as multiple red-purple lesions occurring on the trunk and proximal limbs and have not been reported in patients without POEMS. The formation of glomeruloid hemangiomas is most likely mediated by angiogenic factors. Deposition of immunoglobulins in endothelial cells has also been proposed as a possible triggering mechanism for these lesions. PAS-positive material is found in the cytoplasm of endothelial cells and may represent immunoglobulins derived from the circulation. These hemangiomas may be specific markers for POEMS and their identification may facilitate a more rapid diagnosis. From the Departments of Neurology (T.W., L.G.) and Medicine (A.N.), Robert C. Byrd Health Sciences Center, Morgantown, WV. Disclosure: The authors report no conflicts of interest. February (1 of 2) 2006 NEUROLOGY 66 453 Received September 5, 2005. Accepted in final form October 26, 2005. Address correspondence and reprint requests to Dr. Tracy Weimer, Department of Neurology, Robert C. Byrd Health Sciences Center, Morgantown, WV 26506-9180. Copyright © 2006 by AAN Enterprises, Inc. References 1. Crow RS. Peripheral neuritis in myelomatosis. BMJ 1956;2:802–804. 2. Fukase M, Kakimatsu T, Nishitani H, et al. Report of a case of solitary plasmacytoma in the abdomen presenting with polyneuropathy and endocrinological disorders. Clin Neurol 1969;9:657. Acute trismus associated with Foix–Marie–Chavany syndrome Jennifer A. Frontera, MD; and David Palestrant, MD Foix–Marie–Chavany syndrome is a clinical disorder characterized by faciopharyngoglossomasticatory weakness and loss of voluntary control of facial movements with preserved automatic and emotional motility. It is classically associated with bilateral anterior opercular lesions. Trismus is defined as tonic contraction of the muscles of mastication and can be caused by neuroleptic-induced dystonia, tetanus, basal ganglia disorders, acute infection, idiopathic dystonia, neoplasm, or as a complication of radiation therapy. Though hand dystonia associated with bilateral opercular lesions has been reported,1 trismus associated with Foix–Marie–Chavany syndrome is atypical. We report a patient with trismus and automatic-voluntary dissociation of facial movements after bilateral opercular infarcts. Case report. A 41-year-old right-handed woman, with a history of tobacco use, past cocaine use (⬎10 years ago), and elevated cholesterol, experienced sudden onset dysarthria and left arm and leg numbness and weakness. Her medical history was notable for cryptogenic strokes in the left insula, left temporalparietal, and right frontal territories 5 years prior to admission. Her evaluation at that time included a normal transesophageal echocardiogram (TEE), angiography negative for intracranial stenosis, normal telemetry monitoring, and negative hypercoagulable and vasculitis laboratory studies. The patient was treated initially with warfarin and a statin, but was noncompliant with her medications. She did not receive any neuroleptics prior to or during her hospital stay. Physical examination. Blood pressure was 121/71 mm Hg. Pulse was 62 and intermittently irregular. Respirations were stenorous. The rest of the general examination was unremarkable. Neurologic examination. The patient’s mental status deteriorated within 6 hours of symptom onset from oriented, conversant, and dysarthric to somnolent and intermittently agitated. She demonstrated evidence of left neglect. Cranial nerve examination revealed normal pupils, right gaze preference, and left homonymous hemianopia. The masseter muscles were tonically contracted. She exhibited dysphagia, pooling of secretions, and bifacial weakness with inability to tightly close her eyes or puff her cheeks during spontaneous and emotive facial movement. Assessment of hypoglossal function was impossible given the patient’s trismus. Motor examination revealed left arm and leg plegia with lead pipe rigidity suggestive of dystonia with normal muscle strength on the right. Sensation was decreased to pain on the left face, arm, and leg. Deep tendon reflexes were brisk bilaterally. Because of her trismus and poor mental status, the patient underwent nasal intubation and later tracheostomy. Over the subsequent month the patient improved and was able to move her lips and frontalis muscles both spontaneously and as an emotional response to stimuli. She was able to blink and close her eyes when sleeping, but when instructed to close her eyes, or move her forehead or lips, she was unable to do so. Her masseter muscles remained tonically contracted and the patient was unable to open her mouth either involuntarily or to command. She could communicate by writing and pantomime and had no evidence of aphasia. 454 NEUROLOGY 66 February (1 of 2) 2006 3. Chan JK, Fletcher CD, Hicklin GA, et al. Glomeruloid hemangioma. A distinctive cutaneous lesion of multicentric Castleman’s disease associated with POEMS syndrome. Am J Surg Pathol 1990;14:1036–1046. 4. Tsai CY, Lai CH, Chan HL, Kuo TT. Glomeruloid hemangioma-a specific cutaneous marker of POEMS syndrome. Int J Derm 2001;40:401–414. 5. Vital C, Vital A, Ferrer X, et al. Crow-Fukase (POEMS) syndrome: a study of peripheral nerve biopsy in five new cases. J Periph Nerv Sys 2003;8:136–144. 6. Shahidi O, Myers J, Kvale P. Castleman’s disease. Mayo Clin Proc 1995; 70:969–977. 7. Takatsuki K, Sanada I. Plasma cell dyscrasia with polyneuropathy, organomegaly, and endocrine disorder: clinical and laboratory features of 109 cases. Jpn J Clin Oncol 1983;13:543–556. She required a gastric feeding tube, had copious secretions, and had recurrent aspiration pneumonias. Diagnostic studies. Telemetry revealed evidence of paroxysmal atrial fibrillation. TEE did not reveal a thrombus or patent foramen ovale. Imaging studies. MR diffusion-weighted imaging and apparent diffusion coefficient sequences on day 1 post-stroke revealed patchy acute infarcts in the right insula, opercula, and high parietal and frontal lobes in the MCA territory. T2weighted sequences revealed left opercular, parietal, and right frontal encephalomalacia. There were no basal ganglia, internal capsule, thalamic, or brainstem lesions. Cerebral angiography demonstrated multiple acute branch occlusions of the right rolandic and callosomarginal arteries. The patient was started on warfarin and refused masseter botulinum toxin injection. Figure. Axial MR diffusion-weighted imaging (A) and fluid-attenuated inversion recovery sequences (B) 1 day poststroke and axial CT sections (C, D) 1 week poststroke demonstrate acute patchy right MCA territory infarcts involving the operculum and pre- and postcentral gyrus. Old infarcts of the left anterior operculum and left parietal lobe were present. Discussion. The clinical presentation of facial and pharyngeal weakness accompanied by dissociated automatic and voluntary facial movements with radiographic evidence of anterior opercular lesions is typical of Foix–Marie–Chavany syndrome.2 Supranuclear control of the jaw is largely bilateral, with motor fibers originating in the frontal-opercular area. Our patient was unique in that she developed trismus of acute onset associated with this syndrome. While trismus after stroke has been described with lesions of the basal ganglia, bilateral internal capsules, and brainstem,3,4 it is unusual with bilateral opercular lesions or any of the lesions seen on this patient’s MRI. Additionally, poststroke trismus typically develops subacutely along with spasticity. Our patient developed trismus within 6 hours of symptom onset. Trismus has been successfully treated with botulinum toxin injection into the masseter, temporalis, medial, and lateral pterygoid muscles (figure).3,5 From the Department of Neurology, Division of Stroke and Neurocritical Care, Columbia University College of Physicians and Surgeons, New York, NY. Disclosure: The authors report no conflicts of interest. Received June 16, 2005. Accepted in final form October 27, 2005. Address correspondence and reprint requests to Dr. David Palestrant, Columbia Presbyterian Hospital, 710 W 168th Street, 8th floor, New York, NY 10032; e-mail: [email protected] Copyright © 2006 by AAN Enterprises, Inc. References 1. Puertas I, Garcia-Soldevilla MA, Jimenez-Jimenez FJ, Cabrera-Valdivia F, Jabbour T, Garcia-Albea E. [Bilateral hand dystonia secondary to a bilateral opercular syndrome or Foix-Chavany-Marie syndrome.] Rev Neurol 2002;35:430–433. 2. Foix CCJ, Marie J. Diplegie facio-linguo-masticartrice d’origine souscorticale sans paralys des membres (contribution a l’etude de la localisation des centres de la face du membre superieur). Rev Neurol 1926;33: 214–219. 3. Spillane KS, Shelton JE, Hasty MF. Stroke-induced trismus in a pediatric patient: long-term resolution with botulinum toxin A. Am J Phys Med Rehabil 2003;82:485–488. 4. Lai MM, Howard RS. Pseudobulbar palsy associated with trismus. Postgrad Med J 1994;70:823–824. 5. Kadyan V, Clairmont AC, Engle M, Colachis SC. Severe trismus as a complication of cerebrovascular accident: a case report. Arch Phys Med Rehabil 2005;86:594–595. DO YOU HAVE OLDER NEUROLOGY ISSUES ON YOUR BOOKSHELF? The Neurology Editorial Office is seeking unbound print issues of Neurology from 1951 through the end of 1954 (Volumes 1– 4). These issues are needed because all Neurology content will soon be scanned and then posted on www.neurology.org. From 1951 the journal was published every two months, and in 1954 frequency was increased to monthly. If you have any of these issues that are not bound, please contct the Neurology Editorial Office ([email protected] or 585-275-0816). We will arrange for shipment of these issues. We regret that we will not be able to return the issues to you. We will acknowledge your generous donation in print and online. February (1 of 2) 2006 NEUROLOGY 66 455