Vitiligo: Treatment Approach in Children C E M
Transcription
Vitiligo: Treatment Approach in Children C E M
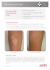
CM E Vitiligo: Treatment Approach in Children Arin L. Isenstein, MD; Dean S. Morrell, MD; and Craig N. Burkhart, MD CM E EDUCATIONAL OBJECTIVES 1. Describe the psychosocial impact of vitiligo in the pediatric population. 2. Identify current treatment options for pediatric vitiligo. 3. Explain the indications for referral of a child with vitiligo to a dermatologist. Arin L. Isenstein, MD, is Resident Physician, Department of Dermatology, University of North Carolina; Dean S. Morrell, MD, is Associate Professor, Department of Dermatology, University of North Carolina; Craig N. Burkhart, MD, is Assistant Professor, Department of Dermatology, University of North Carolina. Address correspondence to: UNC Dermatology, 3100 Thurston-Bowles Bldg., CB#7287, Chapel Hill, NC, 27599-7287; fax 919-966-3898; e-mail aisenste@ unch.unc.edu. Dr. Isenstein, Dr. Morrell, and Dr. Burkhart have disclosed no relevant financial relationships. doi: 10.3928/00904481-20090522-01 V itiligo is a common acquired condition in which the skin and hair become depigmented or hypopigmented. The prevalence of vitiligo ranges between 0.5% and 2% worldwide, and 50% of the cases present before 20 years.1,2 Given the visibility of the disease, vitiligo can have psychological effects including low self-esteem, teasing by others, and social anxiety. Topical therapies and pho- PEDIATRIC ANNALS 38:6 | JUNE 2009 3806Isenstein.indd 339 Figure 1. Acrally distributed vitiligo in areas of trauma. Photos courtesy Dean Morrell, MD. totherapy can safely and effectively repigment the skin and improve quality of life. Here we provide a review of the clinical presentation, epidemiology, associations, pathogenesis, and treatment of vitiligo in the pediatric population. CLINICAL PRESENTATION Vitiligo presents as acquired depigmented or hypopigmented macules of various geographic patterns. It is nonpalpable, not scaly, and asymptomatic. In classic cases, the diagnosis can be www.PediatricSuperSite.com | 339 6/1/2009 4:30:52 PM TABLE 1. Subtypes of Vitiligo in Pediatric Patients Subtypes of Vitiligo Percentage of Cases Generalized (vitiligo vulgaris) 33-78 Focal 14-29 Segmental 4-19 Acrofacial 1-10 Universal Rare TABLE 2. Differential Diagnosis of Vitiligo in a Pediatric Population Tinea versicolor Pityriasis alba Postinflammatory hypopigmentation Lichen sclerosus Nevus depigmentosus Nevus anemicus Tuberous sclerosis Piebaldism made in the primary care setting.3 Often sites of trauma are favored as demonstrated by frequent involvement on the hands, elbows and knees (see Figure 1, page 339). Vitiligo is classified into subtypes based on the pattern and extent of involvement (see Table 1). Generalized vitiligo, also known as vitiligo vulgaris, is the most common type of vitiligo in pediatric patients, ranging from 33% to 78%.2,4-6 These patients have scattered depigmented macules in a symmetric fashion on the face, neck, torso, extensor aspects of extremities, and over bony prominences (Figure 2, see page 341). Focal vitiligo is seen in 14% to 29% of pediatric patients with vitiligo and is defined as localized depigmented macules in a non-dermatomal pattern.2,4-6 Segmental vitiligo, on the other hand, represents localized vitiligo in a dermatomal pattern (Figure 3, see page 342). This type of vitiligo is more common in pediatric patients than in adults and is seen in 340 | www.PediatricSuperSite.com 3806Isenstein.indd 340 4% to 19% of children with vitiligo.2,4-6 Acrofacial vitiligo affects periorificial areas and distal digits. It is less common still, seen in only 1% to 10% of patients.2,4,5 Universal vitiligo refers to the complete depigmentation of the entire skin and is very rare. Trichrome vitiligo describes areas where different degrees of depigmentation create a gradation of skin color (Figure 4, see page 342). In children, vitiligo most often presents first on the head or neck.4,6,7 Other areas of onset in descending order include the trunk, lower extremities, and upper extremities.4,6,7 Often sites of trauma are favored as demonstrated by frequent involvement on the hands, elbows, and knees (Figure 1, see page 339). Mucosal surfaces and hair can also be affected. The differential diagnosis of vitiligo in children is limited (see Sidebar).3 Tinea versicolor, a superficial yeast infection, typically affects the chest and upper back and has a fine scale that can be visualized with lateral pressure applied to the hypopigmented area. Pityriasis alba, illdefined hypopigmented macules, is typically on the face and upper torso of children with atopic dermatitis. Vitiligo of the genitals can be difficult to distinguish from lichen sclerosus, an inflammatory skin condition that causes atrophy. Postinflammatory hypopigmentation results from prior inflammation. These patients will have a history of rash or skin condition localized to and preceding the hypopigmented area. It is extremely rare for vitiligo to present at birth, differentiating it from congenital lesions such as ne- vus depigmentosus, nevus anemicus, ash leaf macules of tuberous sclerosis, and midline depigmentation of piebaldism. EPIDEMIOLOGY The mean age of onset of pediatric vitiligo is 4 to 8 years.2,4,5,7 Some data sets suggest females may be more commonly affected than males, but this difference may reflect a reporting bias.4 Vitiligo affects all races. However, it is more noticeable in darker skinned individuals. A family history of vitiligo is seen in 12% to 35% of pediatric patients with vitiligo,2,4,5,7 with an extended family history of vitiligo being associated with earlier age of onset.6 Affected children are more likely to have a family member with a history of premature graying of the hair, also known as leukotrichia. Additionally, family members are more likely to have autoimmune disorders such as thyroid disease, rheumatoid arthritis, inflammatory bowel disease, alopecia areata, type 1 diabetes mellitus, systemic lupus, multiple sclerosis, and pernicious anemia.2,4,6 Although vitiligo has been associated with a family history of the above autoimmune diseases, no specific autoimmune disorder appears to have a dominant relationship with pediatric vitiligo. There has been much research exploring the association between vitiligo and autoimmune diseases in those affected. In children with vitiligo, concurrent cases of alopecia areata, diabetes mellitus, thyroid disease, Addison disease, and pemphigus vulgaris have been reported.2 In adults, there is an association between vitiligo and autoimmune thyroiditis, also known as Hashimoto’s thyroiditis.8 In children, there may be an association between nonsegmental vitiligo and autoimmune thyroid disease.5,9 Kakarou et al found that children with vitiligo were 2.5 times as likely to develop Hashimoto’s thyroiditis compared to healthy age- and sex-matched controls.5 Based on these findings, annual screening for thyroid dysfunction and autoimmune thyroiditis with a thyroid stimulating hormone, anti-thyroglobulin antibody, and PEDIATRIC ANNALS 38:6 | JUNE 2009 6/1/2009 4:30:53 PM TABLE 2. Therapies for Vitiligo in Pediatric Patients Therapy Potent topical corticosteroids (clobetasol) When and Where to Use Risks - < 20% BSA - Atrophy, striae, telangiectases, hypertrichosis, acne, HPA axis suppression - Face, extremities, torso - < 20% BSA Calcineurin inhibitors (tacrolimus) - Eyelids, face, intertriginous areas Vitamin D derivatives (calciportriene) - In combination with corticosteroids - Burning sensation, malignancy, cost - Segmental vitiligo of head and neck Narrow-band UVB Excimer laser anti-thyroperoxidase antibody has been suggested by some for all children with vitiligo.5 However, other studies have failed to establish an association between autoimmune thyroid disorders and pediatric vitiligo and some pediatric dermatologists screen for autoimmune thyroid disease in asymptomatic patients only if the vitiligo is extensive or there is a strong family history of autoimmune disease.4,10 PATHOGENESIS The pathogenesis of vitiligo is multifactorial. The aforementioned associations of vitiligo with other autoimmune diseases along with detection of antibodies and lymphocytes that recognize melanocyte antigens support an autoimmune etiology.3,11 Other theories include oxidative damage to melanocytes or metabolic derangements within melanocytes leading to apoptosis of these pigment producing cells.12 The histopathology of vitiligo reveals a decreased number or absence of melanocytes in affected skin compared to unaffected skin. TREATMENT Vitiligo is a visible disease that influences quality of life. Young adults with a history of childhood vitiligo reported teasing, being stared at, negative self-image, and feelings of shame.13 Those adults with a history of childhood vitiligo and the aforementioned negative experiences PEDIATRIC ANNALS 38:6 | JUNE 2009 3806Isenstein.indd 341 - > 20% BSA - Cases refractory to topical therapy - Localized disease are more likely to avoid participation in sports, intimacy, and social activities, and have more conflicts with their parents compared with adults with a history of childhood vitiligo who did not report negative experiences.13 Adults with vitiligo reported decreased body-image, self-esteem, and quality of life as well.14 Psychological impact is greater in darker skinned people, women, and when visible areas such as the face and hands are involved.14 Screening patients for psychological effects is recommended.3 We routinely ask our patients and their families how the individual feels about the skin condition and assess if other children are teasing the child. Children and families with psychological concerns can be referred to a specialist for psychological evaluation and counseling. The National Vitiligo Foundation (www.nvfi.org) provides information about local support groups and other resources. After discussion with the patient, no treatment may be considered in patients with fair skin. In these patients, the depigmented areas may not be noticeable and therefore not impact the patient sufficiently to warrant treatment. If repigmentation is not pursued, it is still important to recommend regular sunscreen use as the depigmented areas sunburn easily. For all patients with cosmetically deforming vitiligo, corrective camouflage in the form of foundation and powder - Irritation, cost - Pruritus, dry skin, itching, time-intensive, cost - Redness, blistering, cost Figure 2. Vitiligo vulgaris. Well-demarcated depigmented patches on extensor lower legs. should be offered to cover the depigmented areas. Advice on corrective camouflage can be found at the National Vitiligo Foundation, Dermablend Website (www.dermablend.com), and Cover Fx Web site (www.coverfx.com). Patients with vitiligo who were taught how to apply corrective camoflauge reported substantial improvement in their quality of life.15 Prior to initiating therapy for vitiligo, it is important to discuss expectations. Vitiligo is a chronic skin condition with stable periods and intermittent flares. Spontaneous repigmentation might oc- www.PediatricSuperSite.com | 341 6/1/2009 4:30:53 PM Drug Administration (FDA) approval for the treatment of vitiligo. However, all of the therapies have FDA approval for at least one skin condition in adults or adults and children. Figure 3. Segmental vitiligo. Well-demarcated depigmented patch in a dermatomal distribution. Figure 4. Trichrome vitiligo. Three shades of pigmentation in this early state of vitiligo (same patient as Figure 3 when she presented to our clinic). cur in isolated areas.16 There is no evidence that treating vitiligo influences its chronicity. Although a minority of patients will have 100% repigmentation with treatment, most will not. In most studies, 75% repigmentation defines successful treatment. Certain geographic regions including the head and neck and hair bearing areas are more likely to repigment than others such as the distal extremities.17,18,22 Segmental vitiligo is thought to be more difficult to treat compared to the other subtypes. In patients who pursue treatment, consider subtype of vitiligo, location and extent of involvement when choosing therapy (see Table 2, page 340). Other factors to consider include cost, tolerability, and availability of treatment. No topical therapy has Food and 342 | www.PediatricSuperSite.com 3806Isenstein.indd 342 TOPICAL CORTICOSTEROIDS Potent topical corticosteroids have shown benefit in repigmenting vitiligo in pediatric patients (see Figure 5, page 343). Lepe et al demonstrated 49.3% mean repigmentation with the use of clobetasol (Temovate) 0.05% ointment twice daily for 2 months in a double blind randomized trial.17 Similarly, in a retrospective review of pediatric patients with vitiligo, Cockayne et al reported improvement or resolution of vitiligo in children treated with topical steroids over 2 months to 2 years.18 Repigmentation with topical corticosteroids tends to be most successful on the face and in areas with greater density of hair follicles. The main side effects of topical corticosteroids are atrophy and telangiectases, seen in 15% and 10% of the patients, respectively.17 Hypertrichosis and acneiform eruptions are other known cutaneous side effects of topical corticosteroids. Rarely, hypothalamic pituitary adrenal axis suppression, Cushing’s syndrome, and intracranial hypertension have been reported in children receiving topical corticosteroids.19-21 Potent topical corticosteroids should be considered for treating vitiligo involving less than 20% body surface area or when treatment is focused to cosmetically sensitive areas.22 Regular monitoring for evidence of atrophy, especially in thin skinned areas such as the eyelids, face, and intertriginous areas is advised. Some recommend treatment with potent topical corticosteroids for no more than 2 months.3 Others recommend alternating 6 to 8 week cycles of class I corticosteroids followed by class V corticosteroids.22 Clobetasol is FDA approved for steroid responsive dermatitis in adults but not in children. TOPICAL CALCINEURIN INHIBITORS Tacrolimus (Protopic) is an immunosuppressive that blocks the action of calcineurin leading to deceased transcription of cytokines. Multiple case reports and studies have demonstrated efficacy of tacrolimus in repigmenting vitiligo.17,23-25 Grimes et al reported a series of six patients, including three children, who repigmented with tacrolimus 0.03% and 0.1% applied twice daily.23 In a randomized trial comparing tacrolimus 0.1% ointment with clobetasol 0.05% ointment, areas treated with tacrolimus had a 41.3% mean repigmentation rate.17 Silverberg et al reported a retrospective review of 57 children with vitiligo treated with tacrolimus 0.03% and 0.1% ointment.24 Head and neck lesions were more likely to repigment and repigmented to a greater extent compared to the trunk or extremities. Additionally, 94% of the cases of segmental vitiligo of the head and neck repigmented to some degree with tacrolimus application. Tacrolimus twice daily dosing was more efficacious than once daily dosing. Side effects of tacrolimus include a burning sensation with application, seen in 10% of the patients.17 No atrophy is appreciated. The long term effects of tacrolimus are unknown. Chronic systemic immunosuppression is associated with increased skin cancers and although this association has not been demonstrated with topical tacrolimus, some suggest advising patients being treated with topical tacrolimus to practice sun protection.24 In 2006, topical tacrolimus received a black box warning for a potential cancer risk based on animal studies and case reports. Tacrolimus 0.1% ointment applied twice daily should be considered in the treatment of pediatric vitiligo involving less than 20% body surface area and focused in cosmetically sensitive areas such as the face.3,26 In particular, tacrolimus has a role in the treatment of vitiligo in atrophy sensitive areas such as the eyelids and in segmental vitiligo of the head and neck. Tacrolimus 0.03% ointment is FDA approved in children over PEDIATRIC ANNALS 38:6 | JUNE 2009 6/1/2009 4:30:54 PM the age of 2 with moderate to severe atopic dermatitis. Tacrolimus 0.1% ointment is FDA approved in adults with moderate to severe atopic dermatitis. TOPICAL VITAMIN D DERIVATIVES Vitamin D derivatives such as calcipotriene (Dovonex) and calcipotriol have been studied for the treatment of childhood vitiligo. Vitamin D derivatives have immunomodulating characteristics and may play a role in melanogenesis.27 Chiaverini et al reported 21 of 23 adult and pediatric patients with vitiligo treated with calciportriol in a randomized study had no repigmentation after 3 to 6 months of therapy.28 Conversely, Gargoom et al reported a prospective open label study in which 10 of 18 children with vitiligo treated with calcipotriol twice daily had some degree of repigmentation.29 One patient complained of irritation. Based on these reports along with other studies in adults, the use of vitamin D derivatives as monotherapy for vitiligo is not recommended.3 Combination topical therapy of calcipotriene and corticosteroids for the treatment of pediatric vitiligo may be beneficial. Travis and Silverberg reported a series of 12 patients with pediatric vitiligo treated with topical corticosteroids in the morning and calciportriene in the evening.27 Eighty-three percent of the patients repigmented. Eyelid and facial skin repigmented best and no adverse events were reported. Calcipotriene is FDA approved for the treatment of plaque psoriasis in adults. PHOTOTHERAPY Narrow-band UVB radiation has been studied in children with vitiligo and has a role in repigmentation, especially in patients with greater 20% body surface area affected and in vitiligo refractory to topical treatments.3,30,31 Narrow-band UVB radiation has a spectrum of 310315 nm with a maximum wavelength of 311 nm. Light therapy takes place two PEDIATRIC ANNALS 38:6 | JUNE 2009 3806Isenstein.indd 343 Figure 5. Therapeutic response of segmental vitiligo to topical corticosteroids. to three times a week at the doctor’s office in a phototherapy unit with multiple light bulbs, similar in appearance to a tanning bed in which the patient stands upright. Eye protection is provided, unless eyelids are being treated, in which case the patient keeps his eyes closed. Each treatment lasts a few minutes. The mechanism of action is thought to be multifactorial with narrow-band UVB halting further depigmentation and stimulating melanogenensis. In an open trial, Njoo et al treated 51 children who had a mean affected body surface area of 15% with narrow-band UVB radiation twice weekly.30 Fiftythree percent had greater than 75% repigmentation. Lesions on the face and neck responded best; lesions on the hands, feet, fingers, and toes did not repigment well. In addition to demonstrating repigmentation, the group measured improved quality of life. Similarly, Brazzelli et al reported an open uncontrolled trial of 10 children with vitiligo treated with narrow-band UVB radiation therapy twothree times per week.31 Five patients had greater than 75% repigmentation. Main side effects included itching, dry skin and erythema. No phototoxic or photoallergic reactions have been reported in children being treated with nar- row-band UVB for vitiligo. There is no early increased risk of developing skin cancers in patients treated with narorowband UVB.32 However, long-term studies and studies in children are lacking. Recently, the excimer laser has been shown to be effective in repigmenting focal vitiligo. With a wavelength of 308 nm, the excimer laser provides localized narrow-band UVB. In a retrospective review, 52% of 55 vitiligo lesions in 32 adult and pediatric patients demonstrated greater than 74% repigmentation with 8 to 30 laser treatments.33 As with narrow-band UVB, lesions on the face responded best, while lesions on the hands and feet were least responsive. Darker skinned individuals repigmented more than their lighter skinned counterparts. Initial studies of combination therapy of topical corticosteroids with excimer and tacrolimus with excimer appear superior to excimer laser as monotherapy.34,35 Side effects of the excimer laser include redness and blistering. No studies exploring skin cancer risk and excimer laser have been published. Topical psoralens with both natural sunlight and UVA (topical PUVA), as well as oral psoralens with UVA (oral PUVA) have also been studied for the treatment of vitiligo.36,37 Although effective, psoralens are phototoxic, and patients must www.PediatricSuperSite.com | 343 6/1/2009 4:30:57 PM be counseled to avoid exposure to sunlight beyond the determined treatment time. Additionally, psoralens can cause nausea and itching. In general, oral psoralens are not recommended for children under 12 years of age because of unknown long-term effects. In a recent randomized, doubleblind clinical trial comparing narrow-band UVB with oral PUVA, narrow-band UVB repigmented a greater area, had better color match, and had fewer side effects. With this study, narrow-band UVB supplanted PUVA as the phototherapy treatment of choice for vitiligo given its greater efficacy and superior safety profile. SURGICAL TREATMENT Surgical treatment of vitiligo has not been extensively studied in children and adolescents. A case series of 10 adolescents with 15 patches of vitiligo treated with suction blister epidermal grafts revealed that 86% of the lesions repigmented at least 75%.38 Adolescents had greater repigmentation compared to adults treated similarly. Given the paucity of data on grafting in children, surgical treatment is not a first line therapy in pediatric patients. CONCLUSION Vitiligo is relatively easy to diagnose but difficult to treat. Regular screening of the psychosocial effects of vitiligo and consideration of screening for autoimmune thyroid disease in children and adolescents with vitiligo is recommended. In patients with less than 20% body surface area involved, especially in cosmetically sensitive areas, primary care providers can initiate treatment with either potent topical corticosteroids or tacrolimus. Primary care providers who are uncomfortable using these therapies should refer their patients with vitiligo to a dermatologist. Additionally, patients who fail to respond to topical therapy and those with greater than 20% body surface area involved should be referred to a dermatologist for evaluation and treatment with combination therapy or phototherapy. 344 | www.PediatricSuperSite.com 3806Isenstein.indd 344 REFERENCES 1. Nordlund J. The epidemiology and genetics of vitiligo. Clin Dermatol.1997;15(6):875-878. 2. Halder R, Grimes P, Cowan C, Enterline J, Chakabarti S, Kenney J. Childhood vitiligo. J Am Acad Dermatol. 1987;16(5):948-954. 3. Gawkrodger D, Ormerod A, Shaw L, et al. Guideline for the diagnosis and management of vitiligo. Br J Dermatol. 2008;159:1051-1076. 4. Handa S, Dogra S. Epidemiology of childhood vitiligo: a study of 625 patients from North India. Pediatr Dermatol. 2003;20(3):207-210. 5. Kakourou T, Kanaka-Gantenbein C, Papdopoulou A, Kaloumenou E, Chrousos G. Increased prevalence of chronic autoimmune (Hashimoto’s) thyroiditis in children and adolescents with vitiligo. J Am Acad Dermatol. 2005;53(2):220-223. 6. Pajvani U, Ahmad N, Wiley A, et al. The relationship between family medical history and childhood vitiligo. J Am Acad Dermatol. 2006;55(2):238-244. 7. Cho S, Kang H, Hahm J. Characteristics of vitiligo in Korean children. Pediatr Dermatol. 2000;17(3):189-193. 8. Hegedus L, Heidenheim M, Gervil M, Hjalgrim H, Hoier-Madsen M. High frequency of thyroid dysfunction in patients with vitiligo. Acta Derm Venereol. 1994;74(2):120-123. 9. Iacovelli P, Sinagra J, Vidolin A, Capitnio B, Picardo L. Relevance of thyroiditis and of other autoimmune diseases in children with vitiligo. Dermatology. 2005;210(1):26-30. 10. Halder R. Childhood vitiligo. Clin Dermatol. 1997;15:899-906. 11. Kemp E, Waterman E, Weetman A. Immunological pathomechanisms in vitiligo. Expert Rev Mol Med. 2001;3(20):1-22. 12. Silverberg N, Travis L. Childhood vitiligo. Cutis. 2006;77:370-375. 13. Homan M, Korte J, Grottenhuis M, Bos J, Sprnagers M, van der Veen J. Impact of childhood vitiligo on adult life. Br J Dermatol. 2008;159:915-920. 14. Papdopoulos L, Bor R, Legg C. Coping with the disfiguring effects of vitiligo: a preliminary investigation into the effects of cognitive-behavioural therapy. Br J Med Psychol. 1999;72:385-396. 15. Tedeschi A, Dall’Oglio F, Micali G, Schwartz R, Janniger C. Corrective camouflage in pediatric dermatology. Cutis. 2007;79:110-112. 16. Herane M. Vitiligo and leukoderma in children. Clin Dermatol. 2003; 21:283-295. 17. Lepe V, Moncada B, Castaneda-Cazares J, Torres-Alvarez M, Ortiz C, Torres-Rubalcalva A. A double-blind randomized trial of 0.1% tacrolimus vs 0.05% clobetasol for the treatment of childhood vitiligo. Arch Dermatol. 2003;139:581-585. 18. Cockayne S, Messenger A, Gawkrodger D. Vitiligo treated with topical corticosteroids: children with head and neck involvement respond well. J Am Acad Dermatol. 2002;46(6):964-965. 19. Siklar Z, Bostanci I, Atli O, Dallar Y. An infantile Cushing syndrome due to misuse of topical corticosteroid. Pediatr Dermatol. 2004;21(5):561-563. 20. Ellison J, Patel L, Ray D, David T, Clayton P. Hypothalamic-pituitary-adrenal function and glu- 21. 22. 23. 24. 25. 26. 27. 28. 29. 30. 31. 32. 33. 34. 35. 36. 37. 38. cocorticoid sensitivity in atopic dermatitis. Pediatrics. 2000;105:794-799. Hosking G, Elliston H. Benign intracranial hypertension in a child with eczema treated with topical steroids. Br Med J. 1978;1:550-551. Schaffer J, Bolognia J. The treatment of hypopigmentation in children. Clin Dermatol. 2003; 21:296-310. Grimes P, Soriano T, Dytoc M. Topical tacrolimus for repigmentation of vitiligo. J Am Acad Dermatol. 2002;47(5)798-791. Silverberg N, Lin P, Travis L, Farely-Li J, Mancini A, Wagner A, Chamlin S, Paller A. Tacrolimus ointment promotes repigmentation of vitiligo in children: a review of 57 cases. J Am Acad Dermatol. 2004;51(3):760-766. Kanwar A, Dogra S, Parsad D. Topical tacrolimus for treatment of childhood vitiligo in Asians. Clin Exp Dermatol. 2004;29(6):589-592. Lim H, Hexsel C. Vitiligo: to treat or not to treat. Arch Dermatol. 2007;143(5):643-646. Travis L and Silverberg N. Calciportriene and corticosteroid combination therapy for vitiligo. Pediatr Dermatol. 2004;21(4):495-498. Chiaverini C, Passeron T, Ortonne J. Treatment of vitiligo by topical calcipotriol. J Eur Acad Dermatol Venereol. 2002;12(2):137-138. Gargoom A, Duweb G, Elzorghany A, Benghazil M, Bugrein O. Calcipotriol in the treatment of childhood vitiligo. Int J Clin Pharmacol Res. 2004;24(1):11-14. Njoo M, Bos J, Westerhof W. Treatment of generalized vitiligo in children with narrow-band (tl-01) UVB radiation therapy. J Am Acad Dermatol. 2000;42(2):245-253. Brazzelli V, Prestinari F, Castello M, et al. Useful treatment of vitiligo in 10 children with UVB narrowband (311 nm). Pediatr Dermatol. 2005;22(3)257-261. Hearn R, Kerr A, Rahim K, Ferguson J, Dawe R. Incidence of skin cancers in 3867 patients treated with narrow-band ultraviolet B phototherapy. Br J Dermatol. 2008;159(4):931-935. Hadi S, Spencer J, Lebwohl M. The use of the 308 nm excimer laser for the treatment of vitiligo. Dermatol Surg. 2004;30(7):983-986. Passeron T, Ostovari N, Zakaria W, et al. Topical tacrolimus and the 308 nm excimer laser: a synergistic combination for the treatment of vitiligo. Arch Dermatol. 2004;140(9):1065-1069. Sassi F, Cazzaniga S, Tessari G, et al. Randomized controlled trial comparing the effectiveness of 308 nm excimer laser alone or in combination with topical hydrocortisone 17-butyrate cream in the treatment of vitiligo of the face and neck. Br J Dermatol. 2008;159:1186-1191. Sehgal V, Oral trimethylpsoralen in vitiligo in children: a preliminary report. Br J Dermatol. 1971;85(5)454-456. Atherton D, Cohen B, Knobler E, et al. Phototherapy for children. Pediatr Dermatol. 1996:13(5):415-426. Gupta S and Kumar B. Epidermal grafting for vitiligo in adolescents. Pediatr Dermatol. 2002;19(2):159-162. PEDIATRIC ANNALS 38:6 | JUNE 2009 6/1/2009 4:31:00 PM